MALE INFERTILITY
In a couple who cannot achieve pregnancy, the problem is related to the man in 40% of cases, and to both the man and the woman in 20% of cases.
Male genital physiology
As in women, in men GnRH is secreted from the hypothalamus in a pulsatile (wave-like) manner and stimulates the pituitary gland to secrete FSH and LH hormones. While LH enables testosterone secretion from the Leydig cells in the testes, FSH acts on the Sertoli cells and initiates spermatogenesis (sperm production). Sperm mature in approximately 72 days and are transported to the region where they will be stored in about 14 days.
In the form in which they are produced, sperm have a very weak ability to fertilize.
Before reaching the ejaculation stage, they must be transformed into the fluid called semen. About 60% of the approximately 4 ml volume of semen is produced by a structure called the seminal vesicle. The fluid provided by this vesicle gives semen its final form. Prostatic secretions make up 20% of semen, and this fluid contains sperm, acid phosphatase, and proteolytic enzymes that provide liquefaction (“thinning”). Since the prostate is the organ located at the outermost part, the first fluid expelled during ejaculation is prostatic fluid, and the most viable sperm are found in this fluid.
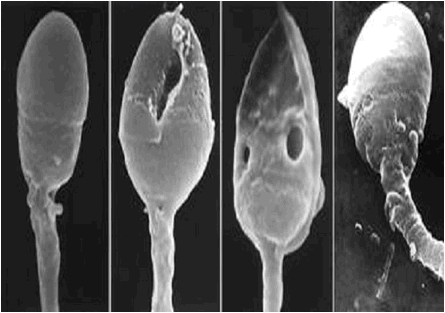
Causes of male infertility
- In male infertility, disorders originating from the testes and neighboring tissues, such as varicocele (dilatation of the veins around the testes), are frequently encountered.
- Disorders of the sperm transport ducts due to gonorrhea and other infections account for 8–10% of cases.
- Hyperprolactinemia and other hormonal disorders are a cause of infertility in about 1% of cases.
- Problems related to sexual intercourse: premature ejaculation, inability to reach orgasm, and impotence (failure of the penis to become erect) are among the less common causes.
- Klinefelter syndrome: this syndrome refers to a chromosomal abnormality of 47, XXY (the normal male karyotype is 46, XY). Due to the extra X chromosome, sperm cannot be produced. It is a rare condition. In mosaic karyotypes (where, in addition to the 47, XXY structure, some cells have a normal chromosomal structure), a small number of sperm may be produced.
- Unknown causes: in a significant proportion of investigations performed for male infertility, no cause can be identified.
Examination and investigations in male infertility
- Urological examination
- Spermiogram (semen analysis)
- Antisperm antibody testing when necessary
- LH, FSH, and prolactin levels when necessary
- Karyotyping (chromosome mapping) to investigate Klinefelter syndrome in suspicious cases
- Genetic testing with chromosomal analysis in cases of azoospermia
- Testicular biopsy: (an advanced investigation performed to search for sperm within the testes in cases of azoospermia, that is, complete absence of sperm)


Comments are closed